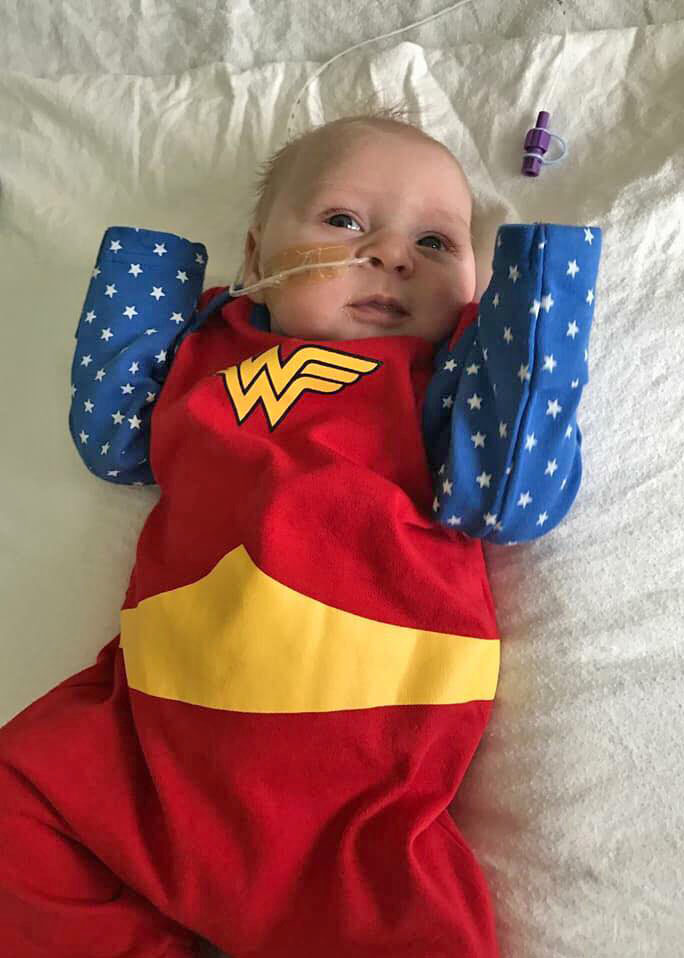
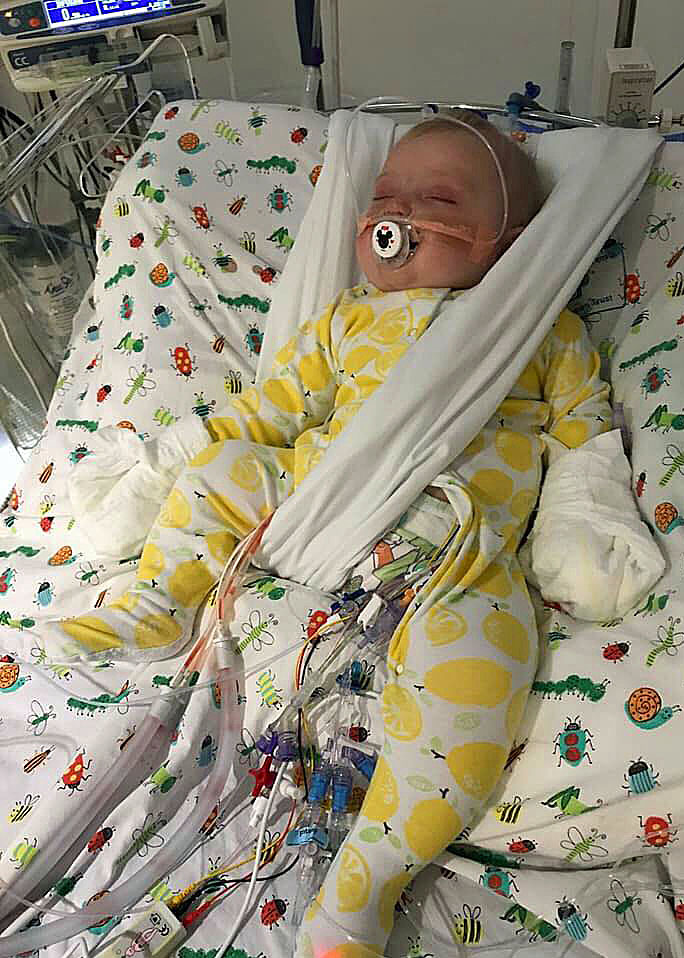
Ivy
Heart Child
20 week scans are exciting. Will you find out or won’t you? Pink or blue? Will you get a clear scan photo? That’s what people focus on when you go for your 20 week scan. We were the same. We’d decided we didn’t want to find out the gender of our baby. We went along, excited, nervous to see our baby again. I was excited as I looked at our baby on the screen for the second time.
The sonographer was talking us through what she could see as she was doing her checks. She was very chatty, asking us if we wanted to know the sex of the baby and then she suddenly went very quiet. I told myself she was just concentrating, that it didn’t mean anything. Those few minutes felt like hours. Her next words cut like a knife, “I’m struggling to get a four chamber view and three vessel view of the heart”. She reassured us and said it could just be how baby if lying but to be on the safe side she wanted us to be scanned by a consultant. The consultant explained that the left side of the baby’s heart looked slender and that the aorta also looked narrow. I couldn’t take it in, I didn’t understand what I was being told. All I took in was that there was an issue with the baby’s heart and that we needed to be referred to foetal medicine for further scans.
Walking out of the hospital I felt numb, I didn’t want to believe what had happened. The following few months involved lots of scans at Liverpool women’s hospital and meetings with the cardiologists from Alder Hey to explain what would happen next. We were given options but we were told that they wouldn’t be able to confirm the exact CHD until after birth. I spent the rest of my pregnancy urging my unborn baby to grow as we were told that the surgery would old take place if the baby was over a certain weight.
We were induced at 39 weeks and after a long labour, Ivy was born on 21st December by emergency C-section. We were both able to hold her and then she was taken to PICU. She was transferred to Alder Hey the next morning whilst I had to stay at Liverpool womens. That was difficult but I was also grateful to get some rest. Later that evening my partner Chris called me to let me know that Ivy had had an echo and that they had confirmed it was the worst case scenario and she had hypoplastic left heart syndrome. She was on prostaglandin to keep the duct in her heart open until they could operate. Not long after hearing this news, I had another phone call telling me that Ivy had been taken to PICU as her blood pressure had dropped and that I needed to get over there. I had only had a c-section that morning but the midwife was happy to discharge me as I could see the midwife at Alder Hey the next day. Luckily Ivy recovered and was back on the ward the next day.
They later spotted on a further echo that she also had a slight leak on the good side of her heart. This hit me like a tonne of bricks as she needed the good side of her heart for the operation to work. On 28th December at just 8 days old Ivy underwent her first open heart surgery and we left her in the hands of her wonderful surgeon Dr Ram. It was the longest day of my life but I was so relieved when we got the phone call to say she was back on PICU and we could go and see her. Dr Ram came out to see us in the waiting area and informed us that the operation had gone well and that Ivy didn’t require ECMO heart support, which we knew was a possibility.
Nothing prepared me for going to see her. She was so swollen, she looked like she’d done 10 rounds with Mike Tyson! Then there were all the lines and machines to warm her up and monitor her and all the alarms. But at the end of the day none of that mattered because our little girl had made it through the first hurdle. It was a slow recovery and she spent until 12th January on PICU and HDU until she was finally allowed back to the ward. But that didn’t last long as on Friday 13th January she took a turn for the worst and was struggling to breathe. Hearing the alarm and seeing people rush into your room was like something out of casualty. It all just felt surreal. They managed to stabilise her and she returned to PICU and was put back on the ventilator.
We were so glad to see two of the nurses we knew when we went back to PICU. Then followed a long slow wean on to C-pap and Optiflow. She had yet another test and it was discovered that she had tracheobronchomalacia, basically her trachea was collapsing when she was breathing. We were told that they would slowly wean her off the oxygen and that at some point she would need a bronchogram but it was likely that she would grow out of it.
The next hurdle we had to face was feeding. Ivy had had an NG tube since birth and although she had taken some bottles she wasn’t taking enough.
It was eventually decided that she would need a PEG to enable her to be able to go home. She had this done on 8th March and we were finally allowed home for the first time on 10th March.
We managed to go on a family holiday with her grandparents, uncles and cousins and we had lots of day trips out around the community nurse visits. Ivy was doing well, she was putting on weight and she was hitting most milestones. We knew that we needed to make the most of this time as she was due to have her second surgery at around 7 months. It felt like we had only just got home from hospital when we received the letter to go for Ivy’s MRI scan.
It was eventually decided that she would have a CT scan and bronchogram whilst under one general anaesthetic. When we got the results back it confirmed that her bronchotraceamalacia was now mild and that she appeared to be growing out of it.
Her next surgery was then scheduled for 10th July, her dad’s birthday. We knew it had to happen and that the risk factors were lower this time but it still didn’t make it any easier. This time she was in Dr Lotto’s hands. I felt surprisingly calm during her second surgery compared to her first.
Again, the phone call came to say she was back on PICU and we could go and visit her. It was so much different the second time round, I was prepared for the lines and alarms but this time she was more awake then previously and had also been taken off the ventilator. She had nappies on her hands and they had to make a sling as she was fighting against the doctors. 6 days after surgery we were allowed home, a little quicker than the 3 months we had spent in hospital after the first surgery.
We still had 3 monthly cardiac clinic appointments and a few weeks on community nurse visits. In December Ivy had her Peg changed to a mic-key button and we went to 6 monthly cardiac clinic visits as her consultant was happy with her.
She is now a happy 15 month old who is hitting her milestones, walking everywhere and is always on the go. We have been able to take her on a family holiday to Disneyland Paris and she is now attending toddler music classes. To look at her, you wouldn’t know she had such a severe heart condition.
Charities such as The Children’s Heart Association have helped provide us with information on our journey and organise great events locally for parents and children with CHD.